A common cause of low back and leg pain is lumbar spinal stenosis.
As we age, our spine also ages. These normal wear-and-tear effects of aging can lead to narrowing of the spinal canal. This condition is called spinal stenosis.
Degenerative changes of the spine are seen in up to 95% of people by the age of 50. Spinal stenosis most often occurs in adults over 60 years old. Pressure on the nerve roots is equally common in men and women.
A small number of people are born with back problems that develop into lumbar spinal stenosis. This is known as congenital spinal stenosis. It occurs most often in men. People usually first notice symptoms between the ages of 30 and 50.
Description
Spinal stenosis occurs when the space around the spinal cord narrows. This puts pressure on the spinal cord and the spinal nerve roots, and may cause pain, numbness, or weakness in the legs.
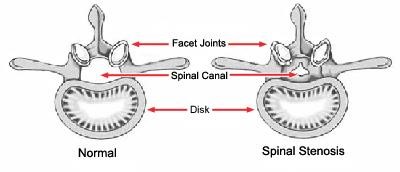
Cause
Arthritis is the most common cause of spinal stenosis. Arthritis refers to degeneration of any joint in the body.
In the spine, arthritis can result as the disk degenerates and loses water content. In children and young adults, disks have high water content. As we get older, our disks begin to dry out and weaken. This problem causes settling, or collapse, of the disk spaces and loss of disk space height.
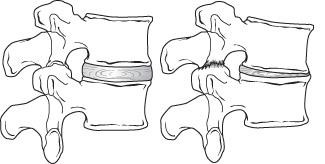
As the spine settles, two things occur. First, weight is transferred to the facet joints. Second, the tunnels that the nerves exit through become smaller.
As the facet joints experience increased pressure, they also begin to degenerate and develop arthritis, similar to that occurring in the hip or knee joint. The cartilage that covers and protects the joints wears away. If the cartilage wears away completely, it can result in bone rubbing on bone.
To make up for the lost cartilage, your body may respond by growing new bone in your facet joints to help support the vertebrae. Over time, this bone overgrowth-called spurs-may narrow the space for the nerves to pass through.
Another response to arthritis in the lower back is that ligaments around the joints increase in size. This also lessens space for the nerves. Once the space has become small enough to irritate spinal nerves, painful symptoms result.
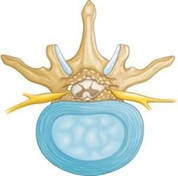
Symptoms
Back pain:- People with spinal stenosis may or may not have back pain, depending on the degree of arthritis that has developed.
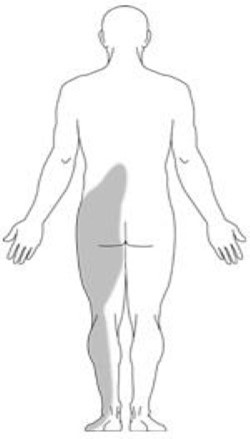
Burning pain in buttocks or legs (sciatica). Pressure on spinal nerves can result in pain in the areas that the nerves supply. The pain may be described as an ache or a burning feeling. It typically starts in the area of the buttocks and radiates down the leg. As it progresses, it can result in pain in the foot.
Numbness or tingling in buttocks or legs. As pressure on the nerve increases, numbness and tingling often accompany the burning pain. Although not all patients will have both burning pain and numbness and tingling.
Weakness in the legs or “foot drop.” Once the pressure reaches a critical level, weakness can occur in one or both legs. Some patients will have a foot-drop, or the feeling that their foot slaps on the ground while walking.
Less pain with leaning forward or sitting. Studies of the lumbar spine show that leaning forward can actually increase the space available for the nerves. Many patients may note relief when leaning forward and especially with sitting. Pain is usually made worse by standing up straight and walking. Some patients note that they can ride a stationary bike or walk leaning on a shopping cart. Walking more than 1 or 2 blocks, however, may bring on severe sciatica or weakness.
Medical History and Physical Examination
After discussing your symptoms and medical history, we will examine your back. This will include looking at your back and pushing on different areas to see if it hurts.
Imaging Tests
X-rays. Although they only visualize bones, X-rays can help determine if you have spinal stenosis. X-rays will show aging changes, like loss of disk height or bone spurs.
X-rays taken while you lean forward and backward can show “instability” in your joints. X-rays can also show too much mobility. This is called spondylolisthesis.
Magnetic resonance imaging (MRI). This study can create better images of soft tissues, such as muscles, disks, nerves, and the spinal cord.
Treatment
Nonsurgical Treatment
Nonsurgical treatment options focus on restoring function and relieving pain. Although nonsurgical methods do not improve the narrowing of the spinal canal, many people report that these treatments do help relieve symptoms.
Physical therapy. Stretching exercises, massage, and lumbar and abdominal strengthening often help manage symptoms.
Lumbar traction. Although it may be helpful in some patients, traction has very limited results. There is no scientific evidence of its effectiveness.
Anti-inflammatory medications. Because stenosis pain is caused by pressure on a spinal nerve, reducing inflammation (swelling) around the nerve may relieve pain. Non-steroidal anti-inflammatory drugs (NSAIDs) initially provide pain relief. When used over a short period, they can also have an anti-inflammatory effect.
These medicines must be used carefully. They can lead to gastritis or stomach ulcers, renal disease.
Steroid injections. Cortisone is a powerful anti-inflammatory drug. Cortisone injections around the nerves or in the “epidural space” can decrease swelling, as well as pain. They also reduce numbness, but not weakness, in the legs. Patients should receive no more than three injections a year.
Surgical Treatment
Surgery for lumbar spinal stenosis is generally reserved for patients who have poor quality of life due to pain and weakness. Patients may complain of difficulty walking for extended periods of time. This is often the reason that patients consider surgery.
Laminectomy. This procedure involves removing the bone, bone spurs, and ligaments that are compressing the nerves. This procedure may also be called a “decompression.” This is a type of open surgery, where the entire back muscles, ligaments are stripped off and the back of the spine is removed to decompress the nerves. It usually requires placement of screws in the spine to stabilise the spine. This leads to prolonged bed rest, delayed mobilisation, increased surgical times, more blood loss, more risk of infection and complications.
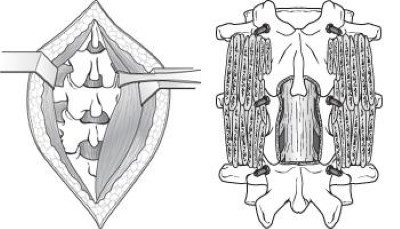
Endoscopic Canal Decompression . This is a modern, advanced stitchless procedure where an small endoscope is introduced in the back and the nerves are decompressed via a key hole incision. This does not cause any muscle stripping, ligament damage and only removes the elements compressing the nerves. This leads to early mobilisation, no need of bed rest, no need of putting screws in the back, minimal blood loss, minimal to zero risk of infection and faster return to daily activities.
Spinal fusion. If arthritis has progressed to spinal instability, a combination of decompression and stabilization or spinal fusion may be recommended. This can also be done via endoscopic approach without causing additional damage to back muscles, ligaments.
Rehabilitation.
We may give you a brace or corset to wear for comfort. We encourage you to begin walking as soon as effects of anethesia wear off. Most patients only need physical therapy to strengthen their backs.
Our physical therapist will teach you exercises to help you strengthen your abdominal muscles, which help support your back.
Most people can go back to a desk job within a few days to weeks after surgery. They may return to normal activities in next 4-6 weeks.
Surgical risks. There are minor risks associated with every surgical procedure. These include bleeding, infection, blood clots, and reaction to anesthesia. These risks are usually very low.
Elderly patients have higher rates of complications from surgery. So do overweight patients, diabetics, smokers, and patients with multiple medical problems.
Specific complications from surgery for spinal stenosis include:
- Tear of the sac covering the nerves (dural tear)
- Failure of the bone fusion to heal
- Failure of screws or rods
- Nerve injury
- Need for further surgery
- Failure to relieve symptoms
- Return of symptoms
Surgical outcomes. Patients tend to see more improvement of leg pain than back pain. Most patients are able to resume a normal lifestyle after a period of recovery from surgery.


